 |
 |
- Search
| Arch Hand Microsurg > Volume 27(3); 2022 > Article |
|
Abstract
Shredder injuries have a poor prognosis and are a problematic type of hand trauma. The authors describe the successful management of two cases of shredder injuries, one involving a child and the other involving an adult. In the child, the authors performed loose skin sutures for closure in the initial surgery and adjusted the degree of intensity of the external compression daily. According to the degree of tissue swelling, the skin sutures were gradually tightened. In the adult, the authors used external compression rather than sutures and adjusted the degree of intensity every day. When treating a shredder injury, the most crucial task is balancing perfusion and tissue pressure to reduce edema while preserving viability, thereby healing and restoring the original function and shape of the injured body part. This paper suggests that external compression may be an important postoperative edema management method in patients with hand shredder injuries.
Shredder machines are currently widely used because they are convenient for tearing or cutting things into thin strips or slices. Unfortunately, accidents have been reported to occur when using these machines, and injuries have been incurred through such mishaps [1,2]. In particular, the prognosis for shredder injuries in hand is not good because such injuries can cause severe through-and-through tissue damage. Even if tissue salvage is possible, the management modality of such injuries is not well known because the number of cases is small. In treating a shredder injury, the most crucial task is balancing perfusion and tissue pressure to reduce edema while preserving viability, thereby healing and restoring the original function and shape of the injured body part. The balancing could be easily achieved with the suture technique in most cases of injuries, but in the case of a shredder injury, the only simple suture technique could reduce perfusion and eventually cause tissue necrosis. Therefore, treatment of a shredder injury is possible if a method of restoring tissue pressure while preserving circulation through external compression, as a complementary and alternative method of suture technique, is used. Although hyperbaric oxygen therapy (HBOT) helps manage shredder injuries [3], not all hand centers can provide it for various reasons. This paper discusses postoperative edema management for successful treatment of shredder injuries based on two cases, one involving a child and the other involving an adult.
This reports was approved from the Institutional Review Board of College of Medicine, The Catholic University of Korea (CMC IRB OC22ZISI0061) and the informed consent was obtained from the patient or the legal guardian for publication of the case report including accompanying images.
A 22-month-old female patient presented with a shredder injury in her left hand by the mushroom shredder, particularly on the index finger to the little finger, accompanied by decreased circulation. There was also a multilevel amputation of the ring finger, and the shredding extended into the ulnar palm (Fig. 1). We set the reconstruction goal as the restoration of the three-point pinch and hand shape due to the severe mutilation of the ulnar ray. Bone fixations with Kirschner wires, multilevel tenorrhaphy, arteriorrhaphy, and neurorrhaphy were performed immediately. As we anticipated severe postoperative swelling, wounds were approximated with loose sutures and covered with fibrin sealant (Tisseel; Baxter, Deerfield, IL, USA) to prevent wound dry-up. A thin foam contact layer (Mepilex Lite; Mölnlycke, Gothenburg, Sweden) and bulky gauze padding distributed gentle compression pressure from the elastic bandage around the hand. In addition, we controlled for severe postoperative swelling by daily tightening the loose skin sutures with #6-0 nylon under anesthesia using intravenous (IV) ketamine, starting from the third to the eighth postoperative day. Finally, the shredded hand survived and regained the three-point pinch function and normal hand shape, except for the ring finger distal phalanx, which had a multi-level amputation.
A 45-year-old female patient presented with a shredder injury on her left middle finger to her little finger by a raw fish shredder (Fig. 2). After thorough wound irrigation, only initial tissue alignment of the mutilated wound was performed rather than suture on the next day of injury because the patient was an adult and had a narrow shred width. Severe edema was observed in the shredded parts, but perfusion was not compromised. After 4 days of surgical delay, we attempted sutures for edema and shape control. However, indocyanine green (ICG) angiography confirmed that suture placement caused poor distal circulation, and restored circulation was observed immediately after suture removal (Fig. 3). Instead of suturing, we attempted to recover tissue pressure through external compression. A thin foam dressing (Mepilex Lite) was rolled around the finger with gentle tension under visualization of fingertip circulation. Finally, the shredded fingers ultimately survived and were restored to their original shapes.
In both the cases mentioned above, we used oxygen supplement using nasal prong and prostaglandin E1; and in case 1, we determined the pediatric drug dose after consulting a pediatric cardiologist.
Shredder injuries can be classified as vertical, oblique, or horizontal, depending on the direction of the damage. In the case of an injury in the horizontal direction, the prognosis is abysmal, and salvage through revascularization is often impossible, resulting in shortening through stump revision. However, better results can be expected in the case of an injury in the oblique direction, especially in the vertical direction.
Effective management of edema is essential for successfully treating upper-extremity trauma [4,5], especially in shredder injuries. Edema has been defined as excess fluid accumulation in the intercellular space. After an injury, protein migrates to an interstitial space due to increased vascular permeability. As osmotic pressure increases, more fluid moves into the interstitial space and aggravates the edema [6]. Persistent edema can lead to a limited range of motion, fibrosis, and scar formation. In addition, posttraumatic contracture induced by edema can result in hand deformities.
Therefore, correcting the imbalance between osmotic and tissue pressure is essential in edema management. Suturing the released compartment and external compression are crucial ways to increase tissue pressure. However, skin necrosis may occur when postoperative edema hinders skin perfusion by tight suturing. Thus, the skin is often sutured loosely at first. In addition, surgeons should consider plasma oncotic pressure maintenance, such as albumin supplements and systemic fluid balance control [7].
In case 2 involving an adult, we tried sutures on the 3rd postoperative day in consideration of surgical delay. Still, intraoperative ICG angiography (on the 4th post-injury day) showed that the circulation was significantly reduced immediately after the suture. Thus, we decided to use external compression rather than sutures, and a hand surgeon adjusted the degree of intensity every day. Too much external compression can cause a decrease in perfusion, so we check the capillary refill of the fingertip for the degree of compression and compress it to just below the maximum degree until the fingertip circulation is maintained. And we also make the compression banding double wound to prevent loosening and compression failure.
In case 1 involving a child, the surgeon performed loose skin sutures during the initial operation and adjusted the degree of intensity of the external compression daily. According to the degree of tissue swelling, the skin suture was gradually tightened on the 3rd to 8th postoperative days, increasing the tissue pressure gradually. This maneuver also reduced the space in which the fluid could accumulate. Adjusting the tension of the sutures is a simple and effective method of reducing postoperative edema in hand, alongside conventional methods such as hand elevation and compressive dressing.
We achieved successful wound healing in the two cases reported herein through external compression only in the adult case and progressive suturing and external compression in the child case. External compression is usually performed for bleeding control in the early stages of trauma. The stronger the compression, the better the hemostatic effect can be expected by decreasing the dead space, increasing the tissue pressure, and causing compression of the damaged vessel. However, conversely, it causes a decrease in circulation, increasing the possibility of causing tissue necrosis. After all, compression is a technique that helps the hemostasis stage, which is the early stage of the acute wound healing process, and an effect equivalent to the primary intention (suture) can be expected. Also, compression is a technique in which the skill of the physician has a great influence on the results. Therefore, if a skilled hand surgeon adjusts the strength of compression every day, an effect comparable to that of a suture in general wound healing can be expected.
HBOT has been reported to help treat shredder injuries [3]. Mechanisms that increase oxygen availability in hypoxic tissue and supplement tissue oxygen tension can be considered suitable for treating shredder injuries [8]. However, in South Korea, the number of medical institutions offering HBOT is significantly smaller than the number of hand centers. Because it is practically impossible to furnish HBOT solely for hand centers for many reasons, such as cost, space, human resources, maintenance, and primarily institutional and health insurance, there should be a careful discussion in adopting this treatment.
ICG angiography offers to be a promising and reliable tool to supplement clinical findings when determining tissue perfusion intraoperatively, as shown in our adult hand shredder injury case [9]. About 3 to 5 mL of dye is injected with a peripheral IV, and tissue fluorescence is examined with a viewing device. Arterial inflow can be assessed with this initial fluorescent reaction. Perfusion examination using ICG angiography can be of great help in the surgeon's decision-making to determine the area to salvage in trauma-induced damage.
Shredder injury forms a flap with a high aspect ratio such that even minor manipulations can easily interfere with distal circulation. Although children could tolerate ischemia in random-patterned flaps more than adults, the shredded flap can easily suffer from disturbances in circulation, even with sufficient surgical delay. Therefore, successful treatment of a shredder injury is possible if a method of restoring tissue pressure while preserving circulation through external compression is used.
Fig. 1.
(A, B) A 22-month-old female patient injured her left hand, particularly on the index finger to the little finger, in a mushroom shredding machine. (C, D) During the initial reconstructive surgery, the wounds were approximated with loose sutures, and the degree of intensity of external compression was adjusted daily. We controlled severe postoperative swelling by tightening the loose skin sutures daily, starting from the 3rd (E, F) to the 8th (G, H) postoperative day. (I, J) Postoperative 4-year follow-up view after release of the first web space contracture with a full-thickness skin graft in the second postoperative year.
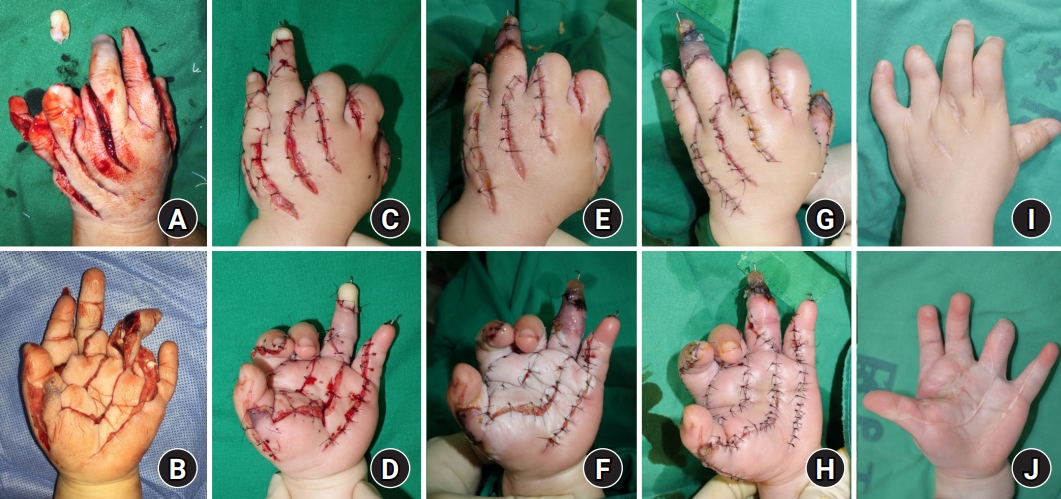
Fig. 2.
(A, B) A 45-year-old female patient injured her third to fifth fingers in a raw fish shredding machine. Only tissue alignment was performed initially. (C, D) Ten-day postoperative view of the wound. Thin foam dressing was rolled around the finger with gentle tension to increase tissue pressure without circulation compromise. (E, F) Ten months after the injury, the shredded fingers survived and were restored to their original shapes through external compression without suturing.
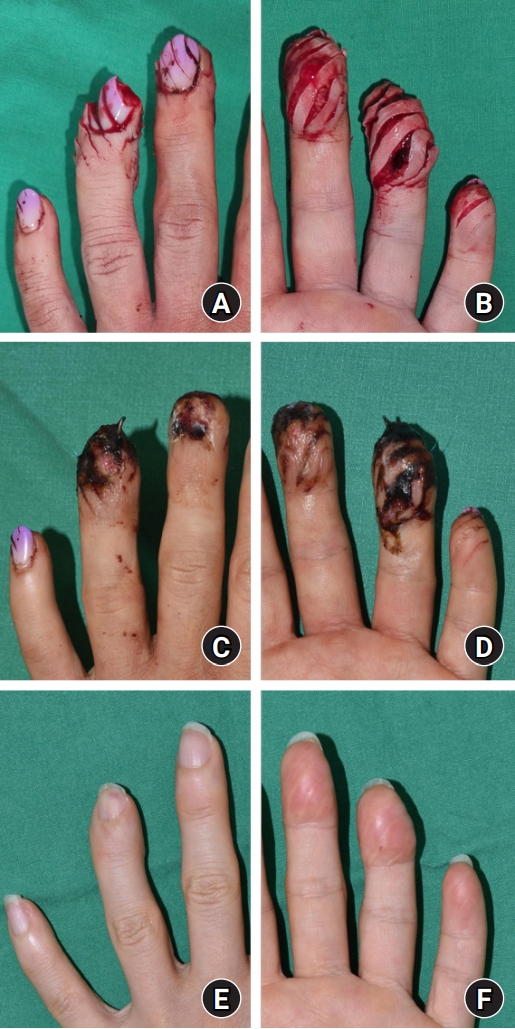
Fig. 3.
(A) After 4 days of surgical delay, only the ring finger’s nail bed (yellow arrowheads), tip, and eponychial folds were sutured. (B) Indocyanine green (ICG) angiography imaging after suturing showed that the sutured flap of the shredding injury had lost contrast due to decreased perfusion. This perfusion difference was more evident when compared to the middle finger's nail bed. (C) ICG imaging after suture removal showed restoration of perfusion by contrast enhancement.

References
1. Brandner M, Bunkis J, Trengove-Jones G. Meat grinder injuries to the upper extremity. Ann Plast Surg. 1985;14:454-7.


2. Warren RC, Foltin GL. Toddlers at risk for paper shredder injury in the home: easy access and severe injury. Pediatrics. 2006;117:535-8.


3. Kim HW, Oh JR. Hyperbaric oxygen therapy and prostaglandin usage for shred injury of the fingers: a case report. Arch Hand Microsurg. 2022;27:54-61.

4. Behnke AR, Forbes HS, Motley EP. Circulatory and visual effects of oxygen at 3 atmospheres pressure. Am J Physiol-Leg Content. 1935;114:436-42.

5. Miller LK, Jerosch-Herold C, Shepstone L. Effectiveness of edema management techniques for subacute hand edema: a systematic review. J Hand Ther. 2017;30:432-46.



6. Howard SB, Krishnagiri S. The use of manual edema mobilization for the reduction of persistent edema in the upper limb. J Hand Ther. 2001;14:291-301.









